
10 Jan 2024
How Sue found hope during AML
Everyone’s leukaemia journey is different. For some, years of gruelling treatment, side effects and relapse require extraordinary mental strength and acceptance.
Therapist Sue Mercer, 71, lives in London with her husband of 44 years, Nick, her dog Dora and cat Rupert. The couple have two sons, Gareth, 43 and Adam, 42.
 “On reflection now I’d had a five or six year history of signs and symptoms that I now know were indicators of leukaemia,” said Sue, who at the time of her diagnosis in 2010 worked as a qualified systemic family therapist and social worker with Islington Childhood and Adolescent Mental Health Service. “I’d had anaemia which was put down to heavy periods and fibroids, night sweats which were attributed to menopause, fungal nail infections, respiratory infections, boils, abscesses, genital herpes and frequent UTIs.”
“On reflection now I’d had a five or six year history of signs and symptoms that I now know were indicators of leukaemia,” said Sue, who at the time of her diagnosis in 2010 worked as a qualified systemic family therapist and social worker with Islington Childhood and Adolescent Mental Health Service. “I’d had anaemia which was put down to heavy periods and fibroids, night sweats which were attributed to menopause, fungal nail infections, respiratory infections, boils, abscesses, genital herpes and frequent UTIs.”
Sue was eventually diagnosed after an appointment with the doctor at the Chelsea and Westminster Hospital who was treating her ongoing hepatitis C. She was referred to haematology after some questionable blood tests although a first bone marrow biopsy showed nothing. A second one revealed that Sue, who was 58 at the time, had acute myeloid leukaemia (AML). She was told the news just before Christmas 2010 and sent immediately to the Catherine Lewis Centre at Hammersmith Hospital for treatment.
“The haematology consultant told me I had 8% chance of survival. I was immediately commenced on Daunorubicin and Cytarabine – chemotherapy. I was told it was gold standard treatment for AML although I misheard this as bog standard and was a bit perturbed!
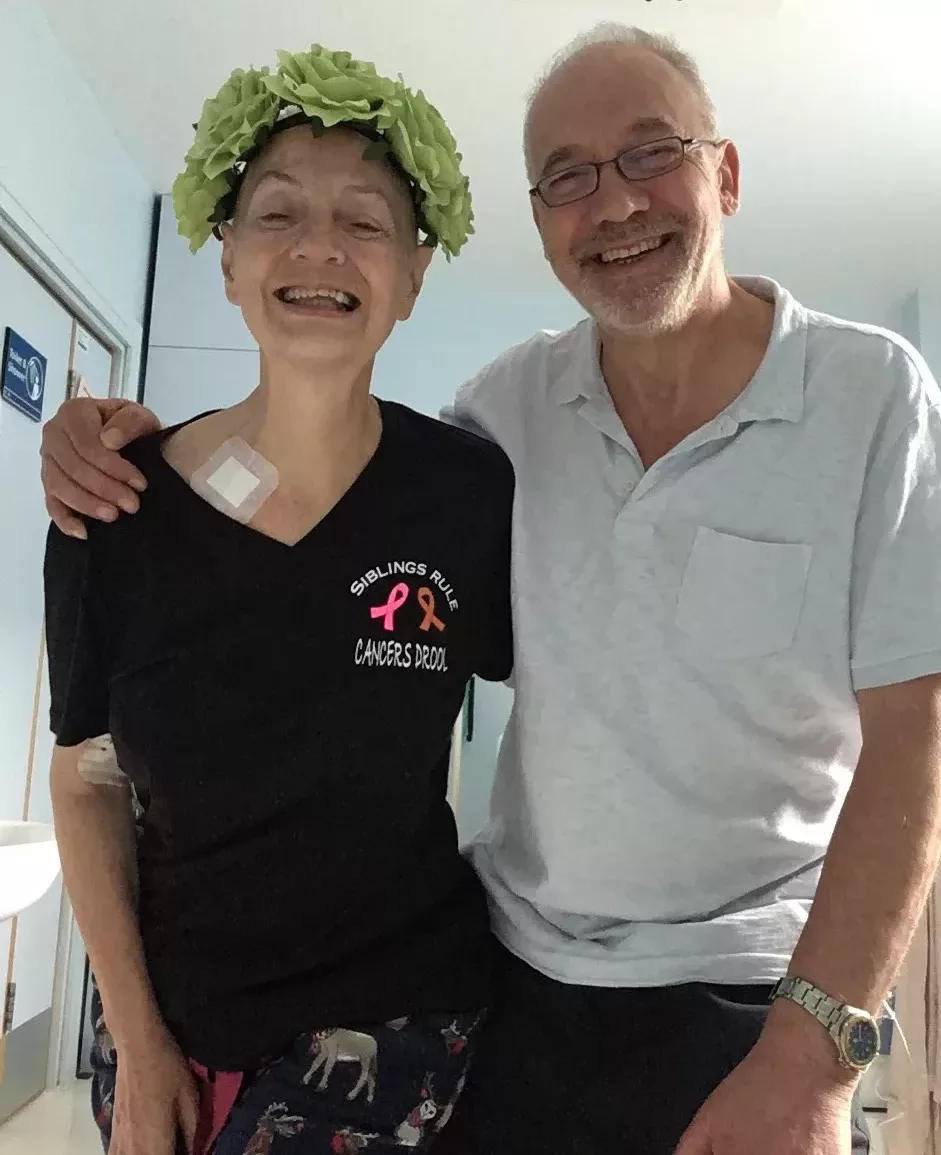 “I’d heard so many horror stories about chemotherapy and looked at alternatives. When we asked my consultant about this he said that those people he knew who went entirely down the alternative route were dead. We agreed to trust the process but at the same time explore other options. I didn’t like the ‘battle’ metaphor and tried to make friends with the chemo.”
“I’d heard so many horror stories about chemotherapy and looked at alternatives. When we asked my consultant about this he said that those people he knew who went entirely down the alternative route were dead. We agreed to trust the process but at the same time explore other options. I didn’t like the ‘battle’ metaphor and tried to make friends with the chemo.”
Sue’s first scheduled discharge was thwarted by an infection. Rather than go home, she eventually opted to stay in hospital and start her second round of chemo. All went smoothly and she was discharged after three weeks. She was sent home officially in remission but told that the AML was likely to return and she would need a stem cell transplant. In July 2011, after a trip to a healing centre in Florida, Sue had her transplant.
“My donor was an Austrian woman in her 30s. I wasn’t able to have any other information but was so moved and grateful.”
In January 2012, six months after the transplant Sue and her husband managed to take a trip to New York. And each 1st July since, the anniversary of her stem cell transplant, they have celebrated her ‘rebirthday’ with trips away to places including Paris and Istanbul.
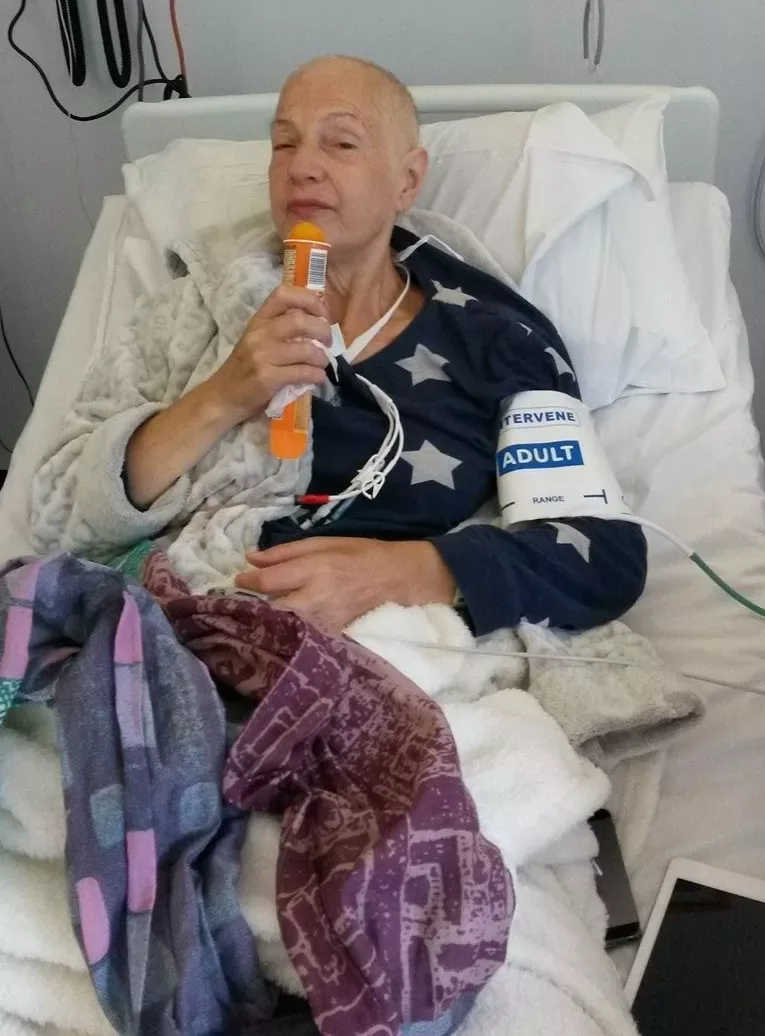 But in May 2017 when she was attending her annual haematology appointment, blood tests revealed her neutrophil count was very low. After a bone marrow biopsy, Sue was told the terrible news that she had relapsed. She was admitted to hospital for chemotherapy, and then, as that didn’t halt her leukaemia, another stem cell transplant. Time was of the essence, and a new donor could not be found, so Sue’s consultant suggested a haploidentical transplant from one of her sons. Both were a 5/10 match and it was agreed her younger son Adam would donate.
But in May 2017 when she was attending her annual haematology appointment, blood tests revealed her neutrophil count was very low. After a bone marrow biopsy, Sue was told the terrible news that she had relapsed. She was admitted to hospital for chemotherapy, and then, as that didn’t halt her leukaemia, another stem cell transplant. Time was of the essence, and a new donor could not be found, so Sue’s consultant suggested a haploidentical transplant from one of her sons. Both were a 5/10 match and it was agreed her younger son Adam would donate.
“I was told I’d get very sick and tried to refuse a nasogastric feeding tube as I’d not got nauseous the first time. But man did I get sick. I’d reluctantly agreed to the tube but the vomiting was so severe the tube was ejected forcibly within 24 hours. I hated the anti-nausea meds that left me feeling like a zombie. I lived on morphine and had horrible dreams. Finally my counts started to rise and with them came Human polyomavirus 1 or BK virus which caused bleeding, painful cystitis.”
Sue was finally discharged home on September 15th 2017 still receiving ongoing treatment for bladder problems. She also had ongoing chest congestion and a blocked nose, and in June developed shortness of breath and a pain in her chest. She was readmitted to Hammersmith Hospital with pericarditis and given strong painkillers and IV antibiotics. Sue had been back home for two weeks after this treatment when she sudden found herself very short of breath. She called an ambulance.
“I was diagnosed with parainfluenza and transferred to my old ward at Hammersmith. Within 12 hours I went into respiratory distress and spent ten days in Intensive Care with respiratory failure. On discharge I weighed 7 stone 12 lbs. My home was adapted as I was unable to climb stairs. I was discharged home Monday August 6th 2018 – the day before my 66th birthday.”
 Sue continued her slow recovery during 2019 but had several hospital admissions to treat what was eventually diagnosed as lung Graft Versus Host Disease and Bronchitis Obliterans Syndrome which was treated with steroids and long term antibiotics. She struggled with depression and anxiety, and was referred for 12 weeks of counselling by her GP. By the time she had her second cataract surgery in February 2020, Sue had gained so much weight on the steroids that it had affected her mobility.
Sue continued her slow recovery during 2019 but had several hospital admissions to treat what was eventually diagnosed as lung Graft Versus Host Disease and Bronchitis Obliterans Syndrome which was treated with steroids and long term antibiotics. She struggled with depression and anxiety, and was referred for 12 weeks of counselling by her GP. By the time she had her second cataract surgery in February 2020, Sue had gained so much weight on the steroids that it had affected her mobility.
2021 was spent having fortnightly Extracorporeal Photopheresis treatment for her GVHD. She also had a spontaneous pelvic fracture and was prescribed morphine. But Sue’s mobility is now improving and she hasn’t had an infection since December 2022. She has been in private psychotherapy for the past three years to help with her mental health.
“In the early days I received a great deal of support on social media. I joined an AML group on Facebook and remain friends with some of the women I met. Throughout my treatment I used complimentary therapies particularly reflexology and acupuncture. I continued with my raw foods diet and used healers, prayers, faith groups – anything that gave me hope. And I kept a journal to the best of my ability.
“We’ve always had cats and these have been a great part of my recovery. Apart from abstaining from cleaning litter trays I’ve taken no other precautions. Becoming a dog owner in 2015 changed our lives for the better. Dora, our cockapoo has been a delight and remains so, encouraging me to take daily walks. And the birth of my grandson in 2011 was a huge milestone in my recovery. I cared for him one day a week until my son and his family moved to Somerset in 2016. We try to visit as often as we can.

“I had my 70th birthday last year. Aging coupled with chronic illness has rendered my body almost unrecognisable. I have struggled with self-image, impacted by steroid belly and hamster cheeks. But over the last year, I’ve started to take small steps towards change. I finally caught Covid and survived with no lingering effects. This gave a huge boost to my confidence and over the last nearly 12 months we’ve ventured out into the world. We’ve taken a few trips to Glastonbury, Liverpool and Fleetwood and we survived despite the fear. Hope has returned.”

Learn about the signs and symptoms of leukaemia.
Related posts
8 September 2022
Statement from Leukaemia UK on the death of Her Majesty Queen Elizabeth II
On behalf of the Leukaemia UK team, Chair of Trustees, Chris Corbin OBE, has made the following statement: “We are extremely saddened to hear the news of the death of…
30 June 2023
New book ‘Bronty’s Battle Cry’ supports Leukaemia UK
‘Bronty’s Battle Cry,’ an inspiring new picture book written by award-winning children’s author and young person’s counsellor, Hannah Peckham, has recently launched and Leukaemia UK are delighted that some of…
16 November 2021
John Goldman Fellowships for 2022 open in December
Leukaemia UK is delighted to continue its investment and funding for early career scientists and clinicians in 2022.
6 March 2024
TV baker Juliet Sear announced as Leukaemia UK Ambassador
Leukaemia UK is excited to announce long-time supporter Juliet Sear as their latest celebrity Ambassador. Juliet, who has been an enthusiastic supporter of Leukaemia UK for several years now, wanted…