11 May 2026
“They said I was just stressed. No one spoke about or did a blood test.”
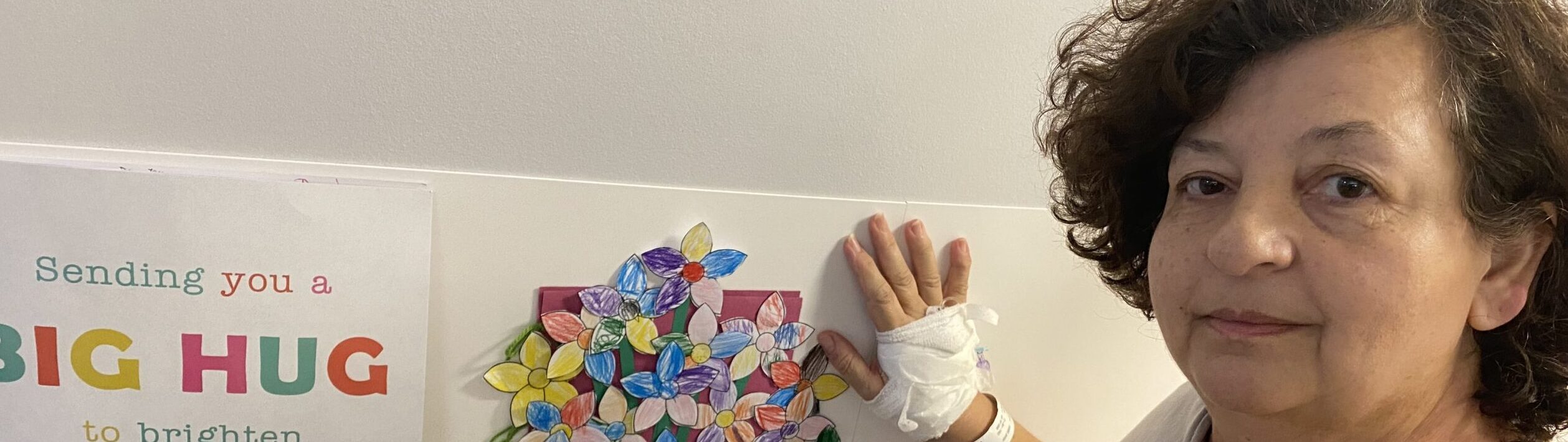
Janev Hakki faced upsetting delays in getting a leukaemia diagnosis which would eventually see her spend nine weeks in hospital undergoing gruelling treatment.
Her symptoms began in October 2023. In her job as a primary school teaching assistant she wa s moved from supporting older children to the reception class and put her tiredness down to the demands of the younger ones.
s moved from supporting older children to the reception class and put her tiredness down to the demands of the younger ones.
“Then I cut my finger and it just wouldn’t heal,” said Janev, 63, who lives in London. “And my thumb turned purple with a huge bruise for no reason.”
“At the beginning of November my symptoms got worse. My left leg went numb and I thought I was developing multiple sclerosis which is what my Mum had passed away from. It was terrifying. I was still going to work every day but decided to go to A&E one evening. They gave me antibiotics but they didn’t work. I got in touch with my GP again and I was advised to go back to A&E. Same thing, antibiotics. They said I was just stressed. No one spoke about or did a blood test.”
By that time Janev was so exhausted she had to cancel spending time with friends and her regular fitness activities. She also developed a huge ulcer on the side of her tongue.
“Then one weekend I was so nauseous and weak I couldn’t get out of bed. I took Monday 29th November off sick, rang 111 and they got the GP to ring me back who said to come and see them as it might be sepsis. I went to my regular surgery but they sent me to Woolwich and said the GP knew I was coming. I paid for an hour on the parking meter and told the receptionist they were expecting me but they said I had to queue. I waited 40 mins in the queue, standing and leaning on the wall, feeling terrible. With five minutes to go on my parking I saw the traffic warden out the window and decided to leave. I thought the doctor would ring me if they were expecting me and sepsis had been mentioned, but they didn’t.”
Eventually Janev got through to the GP and they told her to go to A&E at Queen Elizabeth Hospital in Woolwich. She felt too ill to drive so called her friend Steve.
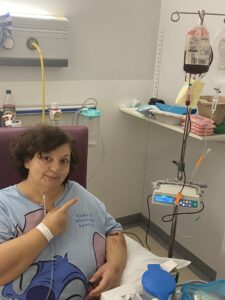 “I couldn’t get out of the car by the time we got there, he had to put me in a wheelchair. We got there at 12noon and they took a blood test, but then I had to wait in the waiting room for the rest of the day. My temperature was over 40 and I couldn’t stop shivering. At 9pm they took me into a stock room. Three doctors came in. They said ‘we’ve got your results back’. Long pause. ‘It’s not good I’m afraid’. I thought they were going to say MS or sepsis. They said ‘I’m afraid you have cancer’. Steve went white with shock. They told me it was blood cancer. If I wasn’t sitting in a wheelchair, I would have collapsed.”
“I couldn’t get out of the car by the time we got there, he had to put me in a wheelchair. We got there at 12noon and they took a blood test, but then I had to wait in the waiting room for the rest of the day. My temperature was over 40 and I couldn’t stop shivering. At 9pm they took me into a stock room. Three doctors came in. They said ‘we’ve got your results back’. Long pause. ‘It’s not good I’m afraid’. I thought they were going to say MS or sepsis. They said ‘I’m afraid you have cancer’. Steve went white with shock. They told me it was blood cancer. If I wasn’t sitting in a wheelchair, I would have collapsed.”
Doctors later confirmed Janev had acute myeloid leukaemia (AML).
“I found out a year later that if I hadn’t had treatment immediately I would have died. At the time I felt like I was dying and was so afraid. They gave me lots of water and kept taking my temperature but I was still in the stock cupboard as they had no where to take me. People were coming in and out taking stock items and I was crying my eyes out.”
After a further wait of around four hours a bed on a general ward was found for Janev and she was put on a drip. A couple of days later she was taken to the MacMillan Cancer Ward and into her own isolation room.
“I was given intravenous antibiotics and other drugs as they confirmed I had sepsis. My temperature was still high. The next day four doctors came to see me and told me that they wanted me to start on a trial drug called Venetoclax. The trial was called The Victor Trial.
The Victor Trial compared two drugs – venetoclax and low dose cytarabine – with intensive chemotherapy. It is for people with AML aged 55 years and older, who the mutation called NPM1.
“I’d told my son Denver by this time and he and Steve asked their work if they could go part time. They were amazing, every day they were there with me.”
Treatment eventually started for Janev on 3rd December once she had recovered from sepsis and would last nine weeks all over Christmas and new year.
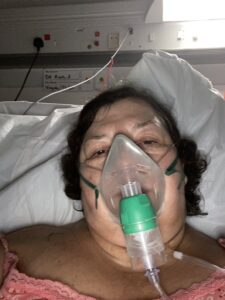 “I had ten consecutive chemotherapy injections in my belly, a blood thinning injection and Venetoclax tablets. The whole experience was just so awful. I felt nauseous, I vomited a lot, I had diarrhoea, I also developed pneumonia and I had a mask to help me to breath, I slept sitting up because I couldn’t breathe if I laid down. I had side affects including cellulitis and vasculitis, my legs were massively swollen and painful. My PICC line also became infected meaning another one had to be put into my other arm which was agony as well. I was allergic to the tape and developed blisters that looked like jelly beans. Emotionally and physically I was drained.
“I had ten consecutive chemotherapy injections in my belly, a blood thinning injection and Venetoclax tablets. The whole experience was just so awful. I felt nauseous, I vomited a lot, I had diarrhoea, I also developed pneumonia and I had a mask to help me to breath, I slept sitting up because I couldn’t breathe if I laid down. I had side affects including cellulitis and vasculitis, my legs were massively swollen and painful. My PICC line also became infected meaning another one had to be put into my other arm which was agony as well. I was allergic to the tape and developed blisters that looked like jelly beans. Emotionally and physically I was drained.
“I also hated the bone marrow biopsies. I had 13 throughout my treatment, once a month at the start. I felt awful the day before, keeping thinking about it. I would shiver and break down.”
After the ninth week, Janev was discharged with chemotherapy injections to give herself at home as well as chemotherapy tablets, blood thinners, anti sickness and other medication. But being an outpatient didn’t last long.
“After taking the first injection at home I went to get up and I collapsed and passed out. I broke my finger as I fell. I managed to call my neighbour who called the ambulance and my son at 8pm. I was taken back to the MacMillan ward and told I would be staying in. I was glad, even though I hated the hospital, because I’d been scared at home on my own.”
After two weeks Janev was sent home again but with regular trips back to the hospital for treatment.
“This went on for most of 2024. I spent more time in hospital that year than I did at home. I had 120 chemo injections altogether.”
Gradually her side effects reduced and she began to recover. After finishing her injections she carried on taking Venetoclax chemotherapy tablets every day for two more years up until March 2026 when she rang the bell at the Macmillan Cancer ward. She still has extreme fatigue but has returned to work as there was no other financial option.

Janev with her friend Steve and her Son Denver and his girlfriend Amelia
“I went back to work full time in September 2025, after a phased return. It was lovely seeing friends and colleagues but all I want to do is get home at the end of the day and go to bed. I love the children but it’s really hard. My joints ache as well, ankles, knee and toes. But it’s not so much the physical it’s the emotional. I’m very tearful. Everything sets me off, I just want to be how I was.
“However I am now thankfully cancer free and in remission. I have to have a blood test every three months and see my consultant. Even though I am in remission, I do worry about a relapse. I know survival rates for AML can be poor and I really want to get to the five-year point.
“Nobody realises or knows how I really feel. Which is so sad. My hopes for the future are to travel again, and I have booked a summer holiday. Whilst on the chemo, I was afraid to go abroad. I loved going to the gym, doing Pilates or body combat, aqua aerobics and taking long walks. I could only go for a gentle swim now. I do exercise and I am trying to get fitter, and I do Rock Choir as well. I get so tired and sleepy and all I want to do is lay down. Because I look ok, everyone thinks that I am.”
Share your story
We want to help people tell and share the leukaemia stories that matter – stories like Janev’s and stories like yours.
Related posts
16 November 2021
Charities call on NHS to treat blood cancer equally in decision-making
The Blood Cancer Alliance undertook an evidence review to inform a new report exploring the unmet needs of people with blood cancer across the UK.
30 June 2023
New book ‘Bronty’s Battle Cry’ supports Leukaemia UK
‘Bronty’s Battle Cry,’ an inspiring new picture book written by award-winning children’s author and young person’s counsellor, Hannah Peckham, has recently launched and Leukaemia UK are delighted that some of…
18 November 2024
Leukaemia UK’s Patient Care Pioneer Award fuels innovative research to revolutionize ‘watch and wait’ approach
Leukaemia UK is excited to announce Professor Francesco Forconi from University Hospital Southampton (UHS) as the first recipient of its Patient Care Pioneer Award. Through this new funding initiative, Professor…
1 August 2022
Pedalling pair’s crazy peaks challenge to stop leukaemia cutting short the lives of beloved mums
Leukaemia UK supporter, Alistair, who lost is mum to leukaemia less than a year ago, is setting out on an extreme fundraising challenge. Alistair, who is from Lincoln, and his…